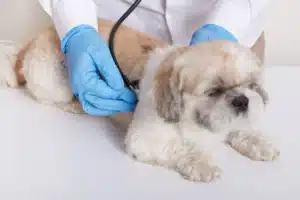
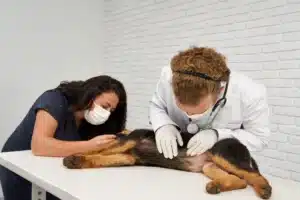
Understanding the oral health, behavior connection changes how we interpret these moments. A dog that stops chewing isn’t being picky, it may be protecting sore gums or sensitive teeth. And snapping during face or muzzle touches is often a pain response, not “bad behavior.” Catching these cues early can help prevent progression to advanced periodontal disease and protect a dog’s comfort and quality of life.
When a normally playful dog suddenly refuses a favorite chew toy, or a friendly companion becomes irritable during petting, many owners blame aging or “mood swings.” But behavior changes caused by dental pain often point to a deeper problem. By age three, an estimated 80–90% of dogs have some degree of periodontal disease. This ongoing inflammation can change how a dog eats, plays, and tolerates touch. In many cases, subtle personality shifts appear before obvious signs like loose teeth, making behavioral awareness an important early warning signal.
Key Takeaways
- Behavior shifts can come first: Dogs may withdraw, refuse chew toys, or change eating habits weeks before owners notice breath odor or gum changes.
- Pain drives personality changes: Irritability, reduced play, social withdrawal, and touch sensitivity are often protective responses to chronic oral discomfort.
- Eating patterns are diagnostic clues: Dropping food, chewing on one side, or eating slowly can signal oral pain even when appetite looks normal.
- Early action reduces long-term damage: Signs like pawing at the mouth or becoming head-shy should prompt a veterinary check before disease becomes irreversible.
- Prevention needs routine care: Daily brushing, VOHC-accepted dental products, and professional cleanings can reduce risk and support long-term wellbeing.
Why Do “Personality Changes” Happen with Periodontal Disease?
Personality shifts in dogs with dental disease are rarely mysterious. They’re often practical adaptations to chronic oral pain. As gum inflammation progresses from gingivitis to deeper periodontal infection, many dogs start making small, protective choices, avoiding chewing, resisting face handling, and disengaging from situations that predict discomfort.
In most cases, the pathway looks like this: plaque (a bacterial biofilm) accumulates on the tooth surface, triggers a local inflammatory response, and can progress below the gumline. Once periodontal pockets develop, infection can damage the periodontal ligament and supporting bone, increasing pain and sensitivity during chewing or touch.
The Pain–Behavior Connection
Cornell’s veterinary guidance describes behavior patterns that can accompany painful periodontal disease, including reluctance to chew, taking longer to finish meals, aggressive behavior when approached, and withdrawal from family interactions.
These reactions generally function as coping strategies:
- Chew avoidance reduces pressure on inflamed gums and sensitive teeth
- Slower eating helps the dog reposition food away from painful areas
- Defensive snapping protects the mouth from contact that hurts
- Withdrawal reduces face-to-face interaction that could trigger pain
These aren’t temperament flaws. They’re often pain-avoidance behaviors—especially when the dog cannot “explain” what hurts.
Chronic Pain Builds Over Time
Unlike a short-term injury, untreated periodontal disease can create persistent discomfort that gradually shifts a dog’s baseline mood and activity. Pain is widely recognized as a driver of behavior change in dogs, and it can show up as reduced play, irritability, and avoidance of handling.
Dogs may protect painful areas by avoiding chewing, reducing play, resisting handling, and disengaging socially-behavior that functions as communication when words aren’t possible.
Clinical takeaway: if a dog’s “personality” changes, dental pain should be high on the differential list, especially in dogs over three years old, when periodontal disease becomes very common.
Periodontal Disease In Dogs: Meaning, Progression, And Why It Matters
Periodontal disease is a progressive inflammatory and infectious condition that affects the tissues supporting a dog’s teeth, including the gums, periodontal ligament, and alveolar bone. It can begin as reversible gingivitis and advance to destructive periodontitis that causes attachment loss, bone loss, pain, and eventual tooth mobility or tooth loss.
How Periodontal Disease Starts: Plaque → Calculus → Infection
The process typically begins with plaque, a bacterial biofilm that forms on tooth surfaces within hours after eating. If plaque is not removed with daily brushing, it can start to harden within about 24 hours and mineralize into calculus (tartar) over the following days. Calculus creates a rough surface that traps more plaque and pushes inflammation deeper under the gumline, accelerating tissue damage.
Periodontal Disease Stages In Dogs (Clinical Staging)
Stage 1 — Gingivitis (Reversible)
Inflammation is limited to the gums, causing redness and mild swelling. There is no attachment loss and no bone involvement at this stage.
Stage 2 — Early Periodontitis (<25% Attachment Loss)
Inflammation extends below the gumline. Shallow periodontal pockets develop with less than 25% attachment loss, and early bone loss may be present.
Stage 3 — Moderate Periodontitis (25–50% Attachment Loss)
Attachment loss progresses to 25–50%, pockets deepen, gum recession becomes obvious, and bone loss increases. Tooth stability may begin to decline.
Stage 4 — Advanced Periodontitis (>50% Attachment Loss)
More than 50% attachment loss occurs with severe bone destruction. Teeth may become loose or be lost, and extractions are commonly required to control pain and infection.
What Vets Need To Diagnose It Correctly
A visual mouth check can spot tartar and gum redness, but it cannot reliably stage periodontal disease, because much of the damage occurs below the gumline. Accurate staging typically requires:
- Periodontal probing to measure pocket depth and attachment loss
- Dental radiographs (x-rays) to detect bone loss and hidden root disease
- Visual assessment to document gum inflammation, recession, calculus load, and tooth mobility
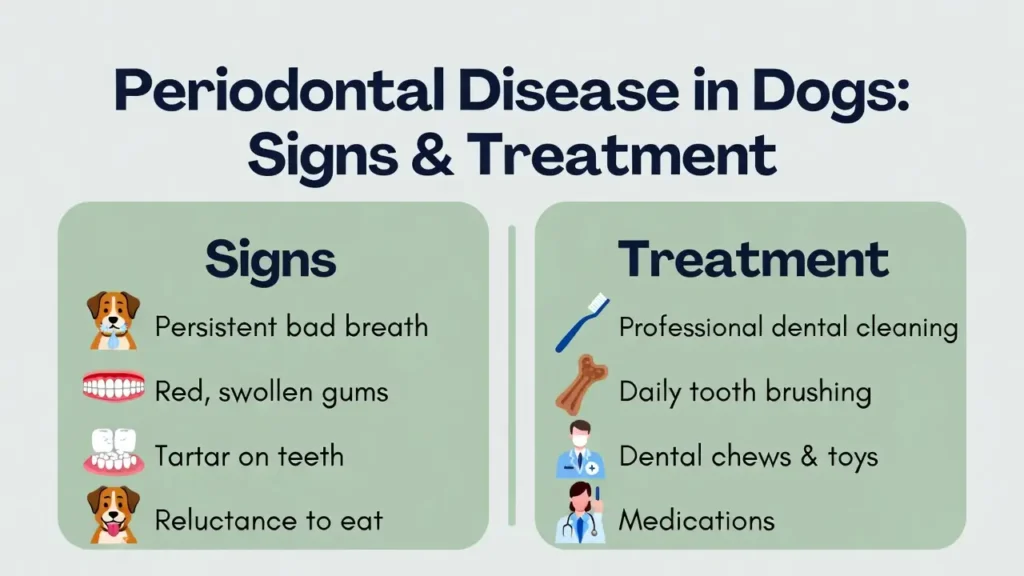
Why Behavior Changes Can Appear Before Visible Dental Signs
Because periodontal destruction often develops under the gumline first, a dog can experience painful periodontal pockets and inflammation before owners notice dramatic tartar buildup or loose teeth. Dogs commonly respond by changing how they chew, how long they take to eat, how much they play, and how tolerant they are of face handling, so behavior may shift earlier than the most obvious visible signs.
How Common Is Periodontal Disease In Real-World Dogs?
Periodontal disease is one of the most common chronic conditions in dogs, but recorded (diagnosed) rates in everyday practice are much lower than the true underlying burden. This mismatch is exactly why early behavioral shifts can be a useful warning signal.
Real-World Diagnosed Prevalence From Primary-Care Records
A large UK primary-care (VetCompass) study based on a random sample of 22,333 dogs reported a 1-year period prevalence of diagnosed periodontal disease of 12.52%.
This number reflects dogs whose periodontal disease was recognized and recorded in that year, not every dog who actually had disease.
True Prevalence Suggested By Clinical Evidence
In contrast, veterinary dental sources commonly report that 80–90% of dogs over the age of 3 have some component of periodontal disease, even when teeth can look “fine” during a casual look.
Taken together, these figures support a practical takeaway: periodontal disease is widespread, and many cases are not formally diagnosed until later.
Why So Many Cases Are Missed Or Diagnosed Late
Several factors explain the diagnostic gap:
- Visual checks miss subgingival disease: A quick look at the teeth cannot reliably show what is happening below the gumline.
- Accurate staging needs probing + dental radiographs: AAHA notes staging is most accurate when performed in an unconscious patient after periodontal probing and intraoral radiographs.
- Radiographs matter even when things look mild: Veterinary guidance emphasizes full-mouth intraoral dental radiographs to avoid overlooking “inapparent” disease.
- Owners normalize early signs: Bad breath and light tartar are often treated as “normal,” which delays professional dental evaluation.
Which Dogs Are At Higher Risk?
Some groups are repeatedly highlighted as higher-risk:
- Small and toy breeds: Cornell notes the problem is worse in smaller breeds (crowding and plaque retention are common contributors).
- Older dogs: Cornell also notes incidence increases with age.
- Breed-related risk in real-world records: The UK primary-care data show breed differences in odds of diagnosis, reinforcing that risk is not evenly distributed.
Behavioral Changes That Appear Before Loose Teeth Are Visible
In dogs with periodontal disease, behavior changes often appear well before owners notice loose teeth or obvious dental damage. These early signs usually affect chewing and play, eating mechanics, and tolerance of facial interaction. Because they precede visible symptoms by weeks or months, they function as some of the most reliable early indicators of oral pain.
Early Changes In Play And Chewing Behavior
One of the earliest warning signs of dental pain is a reduced willingness to chew. Veterinary guidance from Cornell University College of Veterinary Medicine identifies reluctance to chew favorite toys as a common behavioral sign of painful periodontal disease.
Dogs naturally avoid activities that increase pressure on inflamed gums or sensitive teeth, so changes in chewing behavior often follow a predictable pattern.
How Chewing Behavior Evolves As Disease Progresses
Early stages (gingivitis to early periodontitis):
- Shorter chewing sessions with previously favored toys
- Preference for softer chew items over hard or rigid ones
- Reduced excitement when offered chew-based rewards
- Subtle head repositioning while chewing to avoid painful areas
Moderate stages (progressing periodontitis):
- Complete loss of interest in once high-value chew toys
- Avoidance of tug games or jaw-loading play
- Picking up hard chews and dropping them after brief attempts
- Gentle mouthing of toys instead of active chewing
Later stages (moderate to advanced disease):
- Voluntary cessation of chewing activities
- Visible discomfort when biting firm objects
- Carrying toys without attempting to chew
Clinical insight: A sustained reduction in chewing time or intensity with the same toy over several weeks is a strong signal for dental evaluation, even if teeth still appear intact.
Eating Behaviors That Signal Oral Pain Rather Than Picky Eating
Eating changes caused by dental pain differ from ordinary food preferences. Dogs with mouth pain usually remain interested in food but struggle with the mechanics of chewing.
The American Veterinary Medical Association lists abnormal chewing, dropping food, and difficulty eating among common warning signs of dental disease.
Food Handling And Chewing Mechanics
High-signal behaviors associated with oral discomfort include:
- Dropping food while eating, then re-attempting cautiously
- Chewing on one side of the mouth consistently
- Carrying food away from the bowl before chewing
- Tilting the head or adjusting jaw position while eating
Veterinary guidance from Cornell University College of Veterinary Medicine notes that dropping or relocating food before eating may reflect attempts to position it away from painful teeth or inflamed gums.
Changes In Meal Timing And Structure
Dental pain often alters how a dog eats, even when appetite remains normal:
- Taking significantly longer to finish normal portions
- Eating in short bursts rather than one continuous meal
- Approaching the food bowl multiple times before committing to eat
These patterns are commonly described in clinical overviews of canine periodontal disease, including those summarized in the MSD Veterinary Manual.
Texture And Preference Shifts Linked To Mouth Pain
As discomfort increases, many dogs show clear changes in texture tolerance:
- Sudden preference for soft or moistened foods
- Accepting treats but failing to chew or swallow them
- Drinking more water during meals, likely to soften food
These adaptations are consistent with pain-avoidance behavior described in professional dental care guidelines from the American Animal Hospital Association.
How To Differentiate Dental Pain From Picky Eating
The distinction lies in mechanics versus preference:
- Picky eating involves selective interest in certain foods, with normal chewing once eating begins.
- Pain-driven eating involves difficulty chewing regardless of food type.
A dog that eagerly approaches meals but struggles to chew, drops food, or eats unusually slowly is demonstrating oral discomfort, not taste preference.
Why Do Some Dogs Become Irritable, Avoid Touch, Or Seem “Snappy”?
When a dog has painful periodontal disease, irritability around the face is often a protective pain response, not a sudden personality problem. Even gentle dogs may pull away, flinch, growl, or snap when their mouth or muzzle is handled, because contact can trigger sharp discomfort in inflamed gums and tooth-supporting tissues.
How Dental Pain Turns Into Defensive Behavior
Oral pain is unusually disruptive because the mouth is involved in eating, play, grooming, and social contact. When inflamed tissues are pressed or vibrated (petting the muzzle, touching the cheeks, opening the mouth), the nervous system interprets the sensation as a threat and can trigger fast, defensive reactions. Pain is also a well-recognized contributor to “problem behaviors” in dogs, including avoidance and aggression, because the dog is trying to prevent the painful event from happening again.
Over time, many dogs develop anticipatory avoidance: they learn that face handling predicts pain. This learned association commonly leads to a progression of signals:
- Avoidance: turning the head away, ducking, backing up, refusing to be held near the face
- Warnings: lip licking, “whale eye,” pinned ears, stiffening, low growling before contact
- Defensive snapping: a last-resort response if the dog cannot escape and earlier warnings are missed
Cornell’s veterinary guidance lists aggressive behavior when approached as a possible sign when periodontal disease is painful, reinforcing that the behavior can be pain-mediated rather than “dominance” or a training failure.
Situations That Commonly Trigger “Snappy” Moments
Dogs with mouth pain often react most strongly during interactions that involve the head, muzzle, or jaw:
- Head petting and cheek contact (pressure over sensitive structures)
- Collar grabs (force can transmit through the jaw and facial tissues)
- Children leaning into the dog’s face (unexpected, hard-to-avoid contact)
- Grooming around the muzzle (face wiping, beard cleaning, trimming)
- Medication or tooth checks (opening the mouth, touching lips or gums)
A useful pattern clue is location specificity: if a dog tolerates body petting but reacts mainly to face handling, dental pain becomes a high-probability cause compared with generalized anxiety or behavior issues.
How This Affects The Human–Dog Bond
Oral disease can quietly strain daily interaction. Persistent bad breath and discomfort may reduce close contact, cuddling, and playful engagement, and owners can misread avoidance as rejection. Guidance on canine periodontal disease highlights that the condition affects comfort and daily function—so behavior shifts can reflect a quality-of-life problem, not attitude.
Why Do Some Dogs Withdraw From Family Interaction?
Dogs withdraw from family interaction because periodontal disease makes routine social behaviors physically uncomfortable or painful. Everyday family interactions often involve facial contact, food rewards, play, and chewing, all of which can aggravate inflamed gums and painful teeth.
Veterinary guidance from Cornell University College of Veterinary Medicine lists withdrawal from family interaction as a possible behavioral sign when periodontal disease is painful, emphasizing that this change reflects chronic discomfort, not mood or personality shifts.
How Dental Pain Changes Social Behavior
Dental pain alters behavior because dogs learn that social proximity increases the chance of mouth contact or chewing demands. Over time, they reduce interaction to avoid triggering pain.
Observable Social Withdrawal Patterns
Changes in interaction frequency
- Fewer voluntary approaches for affection
- Choosing isolation during busy household activity
- Staying in separate rooms instead of following family members
- Reduced response to name calling or social invitations
Reduced play and engagement
- Declining participation in previously enjoyed games
- Watching family activity from a distance rather than joining
- Reduced excitement during walk or meal preparation
- Avoidance of rough play with other pets
Altered affection-seeking behavior
- Accepting attention but not initiating it
- Moving away after brief petting
- Positioning the body to avoid head or mouth contact
- Loss of “velcro dog” behavior in normally clingy breeds
How To Differentiate Dental Pain Withdrawal From Other Causes
Not all withdrawal is behavioral or emotional. Dental pain has a distinctive pattern that helps differentiate it from anxiety, cognitive decline, or systemic illness.
Key Pattern Differences
| Dental Pain–Related Withdrawal | Other Medical or Behavioral Causes |
| Avoidance focused on face or mouth | Avoidance of all touch |
| Normal tolerance of body contact | Generalized contact avoidance |
| Withdrawal during meals or play | Withdrawal regardless of context |
| Recent onset (weeks to months) | Gradual decline or sudden trauma |
| Eating behavior changes present | Eating patterns unchanged |
Pattern specificity matters:
Withdrawal that centers on activities involving the mouth, while social interest remains partially intact, strongly suggests a dental origin rather than primary behavioral disease.
Which Physical Signs Strengthen The Behavior–Dental Pain Link?
Behavioral changes become far more diagnostic when they appear alongside classic oral signs.The American Veterinary Medical Association lists the following as common indicators of dental disease:
bad breath, abnormal chewing, drooling, dropping food, reduced appetite, and pain around the mouth.

High-Value Clusters That Raise Concern
Oral odor and discharge
- Persistent bad breath with behavior change
- Thick or ropey saliva, sometimes blood-tinged
- Nasal discharge in severe infections
Direct pain indicators
- Pawing at the mouth or rubbing the face on objects
- Teeth chattering or jaw trembling
- Vocalizing when yawning or eating
- Reluctance to open the mouth fully
Visible oral changes
- Red, swollen, or bleeding gums
- Heavy plaque or tartar buildup
- Gum recession exposing tooth roots
- Loose or missing teeth (advanced disease)
Systemic effects
- Reduced appetite or anorexia
- Weight loss in chronic cases
- Lethargy or reduced activity
- Swelling below the eyes (suggestive of tooth root abscess)
Guidance from the MSD Veterinary Manual supports the association between oral pain, chewing difficulty, lethargy, and systemic effects in advanced periodontal disease.
When Does Dental Pain Require Urgent Veterinary Attention?
Seek Immediate Veterinary Care If Any Of The Following Are Present
- Facial swelling or suspected abscess
- Refusal to eat for more than 24 hours
- Bleeding from the mouth
- Severe pain response to gentle face touch
- Sudden onset aggressive behavior
Schedule A Veterinary Exam Within One Week If You Notice
- Progressive difficulty eating
- New refusal of chew toys
- Persistent pawing at the mouth
- Noticeable bad breath plus behavior change
- Visible gum inflammation or tartar buildup
A Practical 2-Minute Home Behavior Screen
This screen compares your dog to its own baseline, not to other dogs.
Step 1: Chew Test (60 seconds)
- Offer a familiar chew item
- Observe engagement: Engage / Hesitate / Avoid
Red flag: shift toward hesitation or avoidance over 2–3 checks
Step 2: First-Bite Check (during next meal)
- Watch the first 10 bites
- Look for dropping food, one-sided chewing, head tilting
Red flag: abnormal mechanics for 3+ meals
Step 3: Touch Tolerance Test (30 seconds)
- Lightly stroke cheek and jawline
- Stop if flinching or avoidance occurs
Red flag: shift from tolerant to sensitive or reactive
Step 4: Social Engagement Observation
- Note approach frequency during normal family activity
Red flag: consistent reduction over 7–14 days
Decision rule:
If two or more categories show persistent change, a veterinary oral exam becomes clinically relevant.
What Can A Veterinarian Confirm That Owners Cannot?
Definitive diagnosis and staging of periodontal disease cannot be done at home.
According to the MSD Veterinary Manual, accurate diagnosis requires periodontal probing and dental radiographs under anesthesia to assess bone loss and attachment damage.
Diagnostic Gold Standard
Periodontal probing
- Measures pocket depth
- Detects attachment loss
- Determines disease stage
Dental radiography
- Reveals bone loss below the gumline
- Identifies root abscesses
- Guides treatment planning
A critical principle emphasized in the American Animal Hospital Association dental guidelines:
visible tartar does not correlate reliably with disease severity.
Why Early Behavioral Detection Matters
Bone loss in Stage 3–4 periodontal disease is irreversible, often requiring extractions. Detecting pain-driven behavior changes during Stage 1–2 allows intervention before permanent damage occurs—preserving comfort, function, and the human–animal bond.
What Prevention Steps Are Most Evidence-Aligned?
Preventing periodontal disease in dogs requires consistent plaque control, regular professional assessment, and judicious use of validated adjunct products. Authoritative veterinary guidelines emphasize that prevention is not optional maintenance, it is the most effective way to reduce pain, tooth loss, and downstream health complications associated with periodontal disease.
The American Animal Hospital Association (AAHA) specifically highlights preventive dental care as essential for minimizing the adverse effects of periodontal disease on canine health.
Daily Plaque Control: The Core of Prevention
Daily mechanical plaque removal is the single most effective preventive measure against periodontal disease. Plaque is a bacterial biofilm that forms on tooth surfaces within hours and begins contributing to inflammation long before tartar becomes visible.
Why Tooth Brushing Matters Most
Veterinary dental research consistently shows that daily tooth brushing can reduce plaque accumulation by up to 90% compared with no brushing. Even brushing several times per week provides measurable benefit, but daily brushing offers the most reliable protection.
Evidence-Aligned Brushing Protocol
- Frequency: Daily (same time each day to build routine)
- Tools: Dog-specific toothpaste and a soft-bristled dog toothbrush or finger brush (never human toothpaste)
- Technique:
- Focus on the outer (cheek-side) tooth surfaces where plaque accumulates most
- Use gentle circular motions at a 45-degree angle to the gumline
- Spend approximately 30–60 seconds total
- Prioritize the back molars, where periodontal disease often begins
- Introduction: Gradual desensitization over 2–3 weeks, starting with finger contact, then toothpaste tasting, then brushing
Professional Dental Cleanings: What Home Care Cannot Replace
Home care alone cannot remove established tartar or assess disease below the gumline. Professional dental cleanings under anesthesia allow veterinarians to perform procedures that are impossible in an awake dog.
What Professional Dental Care Provides
According to the MSD Veterinary Manual, comprehensive dental care includes:
- Scaling above and below the gumline
- Periodontal probing to measure attachment loss
- Full-mouth dental radiographs to detect bone loss and root pathology
- Polishing to smooth enamel and slow plaque reaccumulation
- Treatment planning based on disease stage
Recommended Cleaning Frequency
- Low-risk dogs: Annual dental evaluation; cleaning as indicated
- High-risk dogs (small breeds, seniors, prior disease): Every 6–12 months, based on veterinary recommendation
Adjunct Dental Products: Helpful, but Not Substitutes
When brushing compliance is imperfect, validated adjunct products can provide supplemental benefit.
The Veterinary Oral Health Council (VOHC) evaluates dental products and maintains a list of those shown to reduce plaque and/or tartar.
VOHC-Accepted Product Categories
- Dental chews and treats
- Prescription dental diets
- Water additives
- Oral gels and sprays
- Dental-specific chew toys
Critical caveat:
VOHC acceptance confirms adjunct benefit, not replacement value. These products do not substitute for brushing or professional care, but they can meaningfully support a broader prevention plan.
An Evidence-Aligned Dental Care Routine
A practical, prevention-focused routine integrates multiple layers of care:
Daily
- Tooth brushing (ideal) or VOHC-accepted dental chew
- VOHC-accepted water additive (if used consistently)
Weekly
- Brief behavioral screening (chewing, eating mechanics, touch tolerance)
- Visual oral check for redness, odor, or tartar
Every 6–12 Months
- Veterinary dental examination
- Professional cleaning if indicated
As Needed
- Immediate veterinary assessment for new behavioral signs suggestive of oral pain
Why Some Dogs Require More Aggressive Prevention
Small and Toy Breeds: Elevated Risk
Small dogs experience higher periodontal disease rates due to tooth crowding, retained deciduous teeth, and genetic susceptibility. Cornell University notes that periodontal disease is often more severe in smaller breeds.
Common high-risk breeds include:
Yorkshire Terriers, Chihuahuas, Maltese, Toy Poodles, Pomeranians, Miniature Dachshunds, Shih Tzus
Modified prevention approach
- Begin dental care early (by 1–2 years of age)
- Increase professional cleaning frequency
- Use appropriately sized dental tools
- Monitor behavior changes closely
Senior Dogs: Cumulative Risk and Pain Impact
Dental disease severity increases with age due to cumulative plaque exposure and reduced immune resilience.
Senior dogs also require:
- More thorough pre-anesthetic screening
- Careful pain management
- Greater emphasis on quality-of-life preservation
AAHA guidelines stress that dental pain in senior dogs significantly affects wellbeing and should not be dismissed as “normal aging.”
Breed-Specific Anatomical Challenges
- Brachycephalic breeds: Dental crowding and malocclusion accelerate disease
- Sighthounds: Thin gingival tissue predisposes to recession despite minimal tartar
- Working and hunting dogs: Dental trauma, foreign material exposure, and inconsistent home care increase risk
Why Prevention Matters Beyond the Mouth
Systemic Health Implications
Chronic periodontal infection creates repeated episodes of bacteremia, allowing oral bacteria to enter the bloodstream during chewing. Research links severe periodontal disease with measurable changes in kidney and liver markers in dogs.
While periodontal disease is not the sole cause of organ disease, it is a modifiable risk factor.
Chronic Pain and Quality of Life
Untreated dental pain affects:
- Sleep quality
- Activity levels
- Social bonding
- Mental wellbeing
Dogs often continue eating despite pain, which is why behavioral change—not appetite alone—is a critical signal.
The Predictable Progression of Untreated Disease
Without intervention, periodontal disease typically progresses from gingivitis to advanced destruction over years:
- Stage 1: Gingivitis (reversible)
- Stage 2: Early periodontitis with initial bone loss
- Stage 3: Moderate periodontitis with attachment loss
- Stage 4: Advanced disease with tooth loss and severe bone destruction
Once bone loss occurs, it is irreversible, and treatment focuses on damage control rather than restoration.
Why Early Prevention Is the Highest-Value Intervention
Early intervention:
- Preserves more teeth
- Reduces pain
- Lowers treatment complexity
- Decreases long-term cost
- Prevents systemic complications
Behavioral detection paired with preventive care allows intervention during Stages 1–2, when disease is most manageable and outcomes are best.
Real-World Application: Recognizing Common Behavioral Patterns
Understanding how periodontal disease presents in everyday situations helps owners identify meaningful patterns rather than dismissing early warning signs. The following case patterns illustrate how behavioral changes often precede obvious dental damage.
Case Pattern 1: The Chew-Avoider
Presentation
A three-year-old Miniature Poodle that previously fixated on rope toys suddenly stops chewing over a two-week period. The owner assumes boredom and replaces the toys, but the dog ignores the new ones as well.
Key behavioral signals
- Avoidance of chew toys
- Shortened play sessions
- Normal appetite
- Tolerates general body handling
Veterinary findings
- Moderate tartar accumulation on upper premolars
- Gingival inflammation consistent with gingivitis
- Early periodontal changes (Stage 2) on dental radiographs
Outcome
Professional dental cleaning and initiation of home brushing resulted in full return to normal chewing behavior within one week.
Learning point
Isolated chew avoidance—especially in a young dog with known breed risk—can be an early indicator of periodontal disease, even when other symptoms are absent.
Case Pattern 2: The One-Sided Chewer
Presentation
A seven-year-old Labrador Retriever begins dropping kibble and consistently chewing on the right side of the mouth. Food residue accumulates on the left cheek during meals.
Key behavioral signals
- One-sided chewing
- Dropping food while eating
- Slower meal completion
- Mild avoidance when the left cheek is touched
Veterinary findings
- Fractured upper left carnassial tooth
- Stage 3 periodontal disease surrounding the affected tooth
- Tooth-root abscess detected only on dental radiographs
Outcome
Extraction of the fractured tooth and abscess treatment led to normal bilateral chewing within days.
Learning point
Asymmetric eating behavior is highly suggestive of unilateral oral pain and should prompt immediate dental evaluation.
Case Pattern 3: The Withdrawn Senior
Presentation
An eleven-year-old Chihuahua gradually becomes less social over three months. The dog no longer sleeps with the owner and approaches less frequently for attention.
Key behavioral signals
- Reduced social engagement
- Mild irritability when the face is approached
- Decline in affection-seeking behavior
- Noticeable bad breath accompanying behavior change
Veterinary findings
- Severe tartar accumulation
- Multiple loose teeth
- Advanced periodontal disease (Stage 4) with extensive bone loss
- Halitosis linked to tissue necrosis
Outcome
Multiple extractions and a structured pain-management plan resulted in gradual improvement in social behavior over two to three weeks.
Learning point
In senior dogs, gradual withdrawal combined with oral symptoms often reflects advanced dental disease. Earlier intervention may have prevented extensive tooth loss.
Building an Effective Dental Care Routine
An effective dental care plan must be tailored to individual risk, age, and owner capability. A tiered approach helps align effort with need.
Tier 1: Minimum Standard (All Dogs)
Core components
- Annual veterinary dental examination
- Professional cleaning when recommended
- Daily observation for behavioral or oral changes
- Safe, size-appropriate chew items
Best suited for
Low-risk dogs (large breeds, young adults) when daily brushing is not feasible.
Limitations
Provides baseline protection but may not prevent disease in higher-risk dogs.
Tier 2: Standard Prevention (Recommended for Most Dogs)
Core components
- Tooth brushing daily or at least 4–5 times per week
- Annual or biannual dental examinations
- Professional cleaning as indicated
- Weekly behavioral screening
- VOHC-accepted dental chews as adjunct support
Expected outcome
Meaningful reduction in periodontal disease risk and slower disease progression.
Tier 3: Intensive Management (High-Risk Dogs)
Core components
- Daily tooth brushing without exception
- Dental examinations every six months
- Professional cleanings every 6–12 months
- Weekly documented behavioral screening
- Multiple VOHC-validated adjunct products
- Possible prescription dental diet
- Ongoing veterinary partnership
Best suited for
- Small and toy breeds
- Senior dogs
- Dogs with genetic predisposition
- Dogs with history of rapid disease progression
Expected outcome
Maximum prevention and early detection, though genetic factors may still contribute to disease development.
Customizing the Plan
| Factor | Recommended Adjustment |
| Toy or small breed | Escalate to Tier 3 |
| Age ≥7 years | Increase exam frequency |
| Prior dental disease | Tier 3 + closer monitoring |
| Brushing challenges | Increase professional cleanings |
| Concurrent illness | Coordinate dental care with medical management |
| Working/outdoor dogs | Schedule care around field seasons |
Tracking Progress at Home
Maintaining a simple dental log improves early detection and veterinary communication.
Monthly tracking
- Brushing frequency
- Behavioral screening outcomes
- Changes in eating, breath, or interaction
- Professional care dates and findings
Patterns become clearer when changes are documented rather than recalled.
Conclusion: Behavior as an Early Diagnostic Signal
Behavioral changes are one of the earliest and most underused diagnostic indicators of periodontal disease. Dogs often modify chewing, eating, and social behavior long before owners see loose teeth or severe tartar.
Avoidance of chew toys, one-sided eating, irritability during face contact, or social withdrawal are not personality flaws—they are logical adaptations to chronic oral pain.
Because periodontal disease progresses predictably, intervention during early stages can prevent irreversible damage seen in advanced disease. Behavioral awareness allows owners to act while treatment remains simpler, less invasive, and more effective.
Your dog’s personality isn’t changing—they’re communicating discomfort. Learning to recognize dental pain through behavior ensures that communication leads to timely care and a better quality of life.
Frequently Asked Questions
Can periodontal disease change a dog’s personality?
Yes—periodontal disease can change behavior because chronic oral pain makes dogs avoid chewing, face touch, and social situations.
What are the earliest behavioral signs of dental pain in dogs?
The earliest signs are often chew-toy refusal, shorter play sessions, and subtle avoidance of face handling.
Why does my dog suddenly stop chewing toys?
Many dogs stop chewing to protect sore gums or sensitive teeth, especially when periodontal inflammation makes pressure painful.
Can dental pain make a dog irritable or “snappy”?
Yes—irritability around the face is often a protective pain response, not a temperament problem.
Why does my dog growl or pull away when I touch their muzzle?
Dogs learn that face contact can hurt when gums or teeth are inflamed, so they avoid touch to prevent pain.
Is snapping during petting always aggression?
No—snapping that happens mainly during face or mouth contact is frequently pain-related and should trigger a dental check.
Why is my dog eating slower but still hungry?
Dental pain can make chewing difficult, so dogs take longer to finish meals even when appetite is normal.
Why does my dog drop food while eating?
Dropping food often signals oral discomfort because the dog is struggling to grip, position, or chew without pain.
What does one-sided chewing usually mean?
One-sided chewing often suggests unilateral mouth pain (a painful tooth, gum pocket, or fracture) on the opposite side.
How can I tell picky eating from dental pain?
Picky eating is preference-based, while dental pain shows mechanical difficulty—dropping food, chewing slowly, or chewing on one side.
Why is my dog suddenly avoiding family interaction?
Dogs may withdraw because normal interaction includes face contact, play, and treats—activities that become uncomfortable with dental disease.