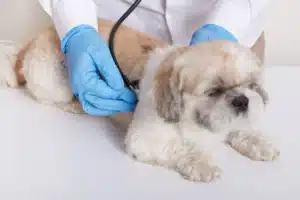
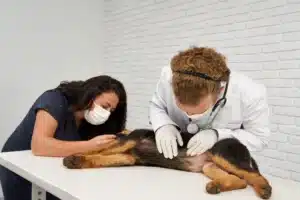
Cushing’s disease in dogs is a chronic endocrine disorder in which the adrenal glands produce excess cortisol, caused by a pituitary tumor in 80–85% of cases and an adrenal tumor in 15–20% of cases. The condition, also named canine hyperadrenocorticism (HAC) or hypercortisolism, affects middle-aged to senior dogs with a median diagnosis age of 10.9 years, according to a 2021 Royal Veterinary College VetCompass study of 905,544 UK dogs published in the Journal of Small Animal Practice.
Cortisol regulates glucose metabolism, immune response, and stress adaptation. Sustained hypercortisolemia triggers polydipsia, polyphagia, polyuria, alopecia, and abdominal distension. The Royal Veterinary College VetCompass study reported a one-year prevalence of 0.17% in UK primary-care practice, with an annual incidence of 0.06%.
This guide covers the causes, symptoms, diagnostic tests, treatment protocols, life expectancy data, and end-of-life care for Cushing’s disease in dogs, based on peer-reviewed veterinary research and primary-care data from 1,527 diagnosed cases.
What Causes Cushing’s Disease in Dogs?
Cushing’s disease in dogs is caused by three distinct mechanisms: pituitary-dependent hyperadrenocorticism (PDH) in 80–85% of cases, adrenal-dependent hyperadrenocorticism (ADH) in 15–20% of cases, and iatrogenic Cushing’s from prolonged corticosteroid therapy.
Pituitary-Dependent Hyperadrenocorticism (PDH)
PDH originates from a functional pituitary adenoma that secretes excess adrenocorticotropic hormone (ACTH), stimulating bilateral adrenal cortical hyperplasia. According to a 2019 University of Bologna epidemiological study of 21,281 dogs published in Open Veterinary Journal, PDH accounts for the majority of spontaneous cases and carries a more favorable prognosis than adrenal-dependent disease.
Adrenal-Dependent Hyperadrenocorticism (ADH)
ADH originates from a unilateral adrenal tumor that autonomously secretes cortisol, suppressing ACTH output. Approximately 50% of adrenal tumors are malignant adrenocortical carcinomas. The remaining 50% are benign adrenocortical adenomas curable through adrenalectomy.
Iatrogenic Cushing’s
Iatrogenic Cushing results from long-term administration of exogenous corticosteroids such as prednisone, prednisolone, or dexamethasone. Chronic exposure suppresses the hypothalamic-pituitary-adrenal axis and mimics spontaneous hypercortisolism clinically and biochemically.
Breed Predisposition
The 2021 VetCompass study at the Royal Veterinary College identified seven breeds with elevated odds of developing Cushing’s disease:
|
Breed |
Odds Ratio (OR) |
95% Confidence Interval |
|
Bichon Frise |
6.17 |
4.22–9.00 |
|
Border Terrier |
5.40 |
3.66–7.97 |
|
Miniature Schnauzer |
3.05 |
1.67–5.57 |
|
Lhasa Apso |
2.52 |
1.49–4.28 |
|
Yorkshire Terrier |
1.82 |
1.23–2.70 |
|
Staffordshire Bull Terrier |
1.52 |
1.08–2.13 |
|
Jack Russell Terrier |
1.50 |
1.07–2.08 |
The same study identified three protected breeds with significantly lower odds: Golden Retrievers (OR 0.24), Labrador Retrievers (OR 0.30), and Border Collies (OR 0.32). Dogs weighing above their breed-sex mean had 1.44 times the odds of diagnosis compared to breed-average peers.
What Are the Symptoms of Cushing’s Disease in Dogs?
The symptoms of Cushing’s disease in dogs are polyuria, polydipsia, polyphagia, bilateral symmetrical alopecia, pot-bellied abdomen, muscle weakness, thinning skin, and recurrent urinary tract infections. Over 80% of affected dogs present with polyuria and polydipsia as the primary clinical signs, according to the Royal Veterinary College VetCompass diagnostic prediction study published in the Journal of Veterinary Internal Medicine (2020).
Eight Primary Symptoms of Canine Cushing’s Disease
- Polydipsia (excessive thirst): Affected dogs drink 2–4 times the normal water intake of 50 mL/kg/day.
- Polyuria (excessive urination): Elevated cortisol impairs renal water reabsorption, producing dilute urine and causing indoor accidents.
- Polyphagia (increased appetite): Cortisol stimulates appetite centers, causing food-seeking behavior and scavenging.
- Bilateral symmetrical alopecia: Hair thins across the trunk, flanks, and tail base while the head and limbs are often spared.
- Pot-bellied appearance: Abdominal distension results from hepatomegaly, fat redistribution, and weakened abdominal musculature.
- Muscle weakness: Cortisol-induced protein catabolism causes muscle atrophy, stair-climbing difficulty, and exercise intolerance.
- Thin skin and calcinosis cutis: Skin becomes fragile, bruises easily, and develops mineralized plaques in chronic cases.
- Recurrent infections: Cortisol-mediated immunosuppression predisposes dogs to urinary tract infections, pyoderma, and otitis externa.
Advanced and End-Stage Symptoms
End-stage Cushing’s disease produces severe lethargy, collapse episodes, uncontrolled urinary incontinence with perineal dermatitis, neurological signs from expanding pituitary macroadenomas, concurrent diabetes mellitus, and systemic hypertension. Calcinosis cutis increases mortality risk 5.27-fold, according to a 2022 prognostic study of 91 dogs published in Veterinary Record.
How is Cushing’s Disease Diagnosed in Dogs?
Cushing’s disease in dogs is diagnosed through the ACTH stimulation test, low-dose dexamethasone suppression test (LDDST), urine cortisol-to-creatinine ratio (UCCR), abdominal ultrasound, and routine bloodwork showing elevated alkaline phosphatase (ALKP) and low urine specific gravity (USG). No single test confirms the diagnosis, and the American College of Veterinary Internal Medicine consensus recommends combining two tests plus imaging.
Diagnosis is complex because clinical signs overlap with diabetes mellitus, chronic kidney disease, and hypothyroidism. The VetCompass study reported that 78.6% of diagnosed cases used the ACTH stimulation test and 28.9% used the LDDST.
Diagnostic Test Comparison
|
Test |
Purpose |
Sensitivity |
Clinical Notes |
|
ACTH Stimulation Test |
Measures cortisol response after synthetic ACTH injection |
57–95% |
First-line screen for iatrogenic cases and the sole test for monitoring trilostane therapy |
|
LDDST (Low-Dose Dexamethasone Suppression) |
Assesses cortisol suppression after 0.01 mg/kg dexamethasone IV |
85–100% |
Higher sensitivity for spontaneous PDH; lower specificity in concurrent illness |
|
UCCR (Urine Cortisol:Creatinine Ratio) |
Screens morning urine sample collected at home |
75–100% |
Useful rule-out test; high false-positive rate in stressed or ill dogs |
|
Endogenous ACTH |
Differentiates PDH from ADH |
Confirmatory |
Elevated in PDH, suppressed in ADH |
|
Abdominal Ultrasound |
Evaluates adrenal gland size, symmetry, and mass |
Anatomical |
Identifies unilateral adrenal tumors and distinguishes PDH from ADH morphologically |
|
CT / MRI of Pituitary |
Detects pituitary macroadenomas |
Anatomical |
Recommended when neurological signs or tumor diameter >10 mm is suspected |
The VetCompass Cushing’s Diagnostic Prediction Tool, developed by Dr. Imogen Schofield and the Royal Veterinary College team, uses 10 predictive factors to estimate disease probability before confirmatory testing. The tool is freely accessible to primary-care veterinarians.
What Treatment Options Are Available for Cushing’s Disease in Dogs?
Cushing’s disease in dogs is treated with trilostane (first-line medication), mitotane (second-line adrenolytic), surgical adrenalectomy for adrenal tumors, radiation therapy for large pituitary tumors, and gradual corticosteroid tapering for iatrogenic cases. Trilostane delivers an 11% higher 36-month survival rate compared to mitotane, according to a 2025 systematic review and meta-analysis of 295 dogs published in the journal Animals.
1. Trilostane (Vetoryl®) — First-Line Therapy
Trilostane is a competitive inhibitor of the 3β-hydroxysteroid dehydrogenase enzyme system, blocking cortisol synthesis in the adrenal cortex. The FDA approved Vetoryl® in 2008 as the only licensed treatment for canine hyperadrenocorticism in the United States.
- Dosing: Twice-daily low doses of 0.2–1.1 mg/kg improve symptom control compared to once-daily regimens.
- Onset of action: Clinical improvement appears within 2–4 weeks.
- Monitoring: ACTH stimulation tests at 10–14 days, 30 days, 90 days, and every 3 months thereafter.
- Adverse effects: Diarrhea, vomiting, and lethargy occur in up to 63% of dogs but are usually mild and self-limiting.
- Rare complications: Iatrogenic hypoadrenocorticism and adrenal necrosis.
See also: Trilostane for Dogs with Cushing’s Disease — Dosage, Side Effects & Results
2. Mitotane (Lysodren®) — Adrenolytic Therapy
Mitotane selectively destroys the zona fasciculata and zona reticularis of the adrenal cortex through cytotoxic action. The drug was the standard treatment before trilostane approval and remains an option for dogs intolerant to trilostane.
- Induction dose: 25–50 mg/kg/day divided BID for 7–14 days.
- Maintenance dose: 25–50 mg/kg weekly.
- Median survival: 708 days (range 33–1399 days) in comparative studies.
- Drug interaction: Phenobarbital accelerates mitotane metabolism; alternative anticonvulsants such as levetiracetam or potassium bromide should be used concurrently.
3. Surgical Treatment
- Adrenalectomy: Curative for benign unilateral adrenal tumors when performed by boarded surgeons at referral centers.
- Transsphenoidal hypophysectomy: Removes the pituitary adenoma directly and is performed at specialty institutions including Utrecht University and UC Davis.
4. Radiation Therapy
Stereotactic radiation therapy treats pituitary macroadenomas exceeding 10 mm in diameter or tumors causing neurological deficits. Radiation shrinks tumor volume, reduces ACTH hypersecretion, and extends survival.
5. Adjunct Supportive Care
- Dietary management: Low-fat, moderate-protein, high-fiber veterinary diets preserve lean muscle mass and reduce hepatic workload.
- Melatonin and lignans: May benefit atypical Cushing’s (sex-hormone Cushing’s) cases under veterinary supervision.
- Omega-3 fatty acids: Support skin integrity and reduce inflammation.
See also: Melatonin for Dogs with Cushing’s Disease — Dosage & Benefits
What Foods and Natural Remedies Help Dogs with Cushing’s Disease?
Dogs with Cushing’s disease benefit from a diet containing less than 12% fat on a dry-matter basis, 18–25% protein from lean sources, and 5–10% fiber to stabilize blood glucose and preserve muscle mass. Diet does not replace trilostane therapy but reduces secondary complications such as pancreatitis and obesity.
Recommended Dietary Components
- Lean animal proteins: Turkey breast, white fish, and egg whites provide essential amino acids with minimal fat.
- Soluble fiber sources: Canned pumpkin, green beans, and psyllium husk improve satiety and glycemic control.
- Low-fat prescription diets: Hill’s i/d Low Fat, Royal Canin Gastrointestinal Low Fat, and Purina EN Low Fat meet published targets.
- Omega-3 fatty acids: Fish oil at 40 mg/kg EPA+DHA daily supports skin, coat, and joint health.
Supplements with Clinical Evidence
- Melatonin: Dosed at 3–6 mg every 12 hours for dogs over 15 kg; used for alopecia X and atypical Cushing’s.
- Flaxseed lignans (SDG): Dosed at 1 mg/lb body weight daily; may reduce sex-hormone excess.
- SAMe and silymarin: Support hepatic function in dogs with elevated ALKP.
Supplements require veterinary clearance because interactions with trilostane and concurrent medications are documented.
How Much Does Cushing’s Disease Treatment Cost?
Cushing’s disease treatment costs $50–150 per month for trilostane, $100–200 per ACTH stimulation test every 3 months, $2,000–6,000 for adrenalectomy surgery, and $2,000–5,000 for stereotactic radiation therapy. Annual outpatient medical management typically costs $1,200–2,500 in the United States.
|
Treatment |
Cost Range (USD) |
Frequency |
Total First-Year Cost |
|
Trilostane (Vetoryl) |
$50–150 |
Monthly |
$600–1,800 |
|
Mitotane (Lysodren) |
$50–120 |
Monthly |
$600–1,440 |
|
ACTH Stimulation Test |
$100–200 |
Every 3 months |
$400–800 |
|
LDDST (diagnostic) |
$200–400 |
One-time |
$200–400 |
|
Abdominal Ultrasound |
$300–600 |
Annually |
$300–600 |
|
Adrenalectomy Surgery |
$2,000–6,000 |
One-time |
$2,000–6,000 |
|
Stereotactic Radiation |
$2,000–5,000 |
One-time |
$2,000–5,000 |
|
Prescription Diet |
$70–120 |
Monthly |
$840–1,440 |
What Is the Life Expectancy of Dogs with Cushing’s Disease?
Dogs with Cushing’s disease treated with trilostane live a median of 662–998 days (approximately 1.8–2.7 years) after diagnosis, while untreated dogs typically survive 6–24 months. A 2022 Veterinary Record study of 91 dogs on twice-daily low-dose trilostane reported a median survival of 998 days (95% CI 755–1241 days, range 26–1832 days).
Published Survival Data by Treatment Protocol
|
Study |
Sample Size |
Median Survival (days) |
Protocol |
|
Neiger et al., 2002 |
78 dogs |
549 |
Once-daily trilostane |
|
Barker et al., 2005 |
123 dogs |
662 |
Once-daily trilostane |
|
Alenza et al., 2006 |
43 dogs |
930 |
Twice-daily trilostane |
|
Arenas et al., 2014 |
40 dogs |
900 |
Twice-daily trilostane |
|
García San José et al., 2022 |
91 dogs |
998 |
Low-dose twice-daily trilostane |
|
Clemente et al. (mitotane comparison) |
25 dogs |
708 |
Mitotane |
Survival by Disease Type
- Pituitary-dependent (PDH): Median survival of 662–998 days with trilostane; 2-year survival rate exceeds 74%.
- Adrenal-dependent benign (ADH): 2–3+ years with surgical adrenalectomy; potentially curative.
- Adrenal-dependent malignant: 6–18 months due to metastatic progression to liver and lungs.
- Iatrogenic Cushing’s: Variable; depends on the primary disease requiring steroid therapy.
- Untreated spontaneous Cushing’s: 6–24 months with progressive symptom burden.
Prognostic Factors
The 2022 García San José study identified four independent predictors of shorter survival: advanced age at diagnosis (HR 1.337), presence of calcinosis cutis (HR 5.271), body condition score ≤3/9, and concurrent diabetes mellitus. A 2023 Research in Veterinary Science study reported that dogs with concurrent Cushing’s and diabetes mellitus had a median survival of 892 days compared to 1,245 days for Cushing’s alone (P = 0.002).
See also: Cushing’s Disease Stages, Treatment Response & Prognosis
What Are the Final Stages of Cushing’s Disease in Dogs?
The final stages of Cushing’s disease in dogs present persistent lethargy, uncontrolled urinary incontinence with skin ulceration, severe muscle wasting, neurological decline from pituitary tumor expansion, and refusal to eat. At this stage, most dogs no longer respond to trilostane dose adjustments or additional therapy.
Seven Clinical Markers of End-Stage Cushing’s
- Persistent lethargy lasting more than 7 consecutive days.
- Collapse episodes during brief activity or rest.
- Urinary incontinence with secondary perineal dermatitis.
- Muscle wasting with inability to stand without assistance.
- Neurological decline including seizures, circling, and disorientation.
- Complete anorexia unresponsive to appetite stimulants.
- Withdrawal from family interaction and loss of behavioral engagement.
See also: Final Stages of Cushing’s Disease in Dogs — Signs & Timeline
How Does Cushing’s Disease Affect a Dog’s Quality of Life?
Cushing’s disease reduces a dog’s quality of life through polyuria-related housetraining breakdown, muscle weakness limiting mobility, skin infections requiring repeated antibiotic courses, and fatigue from cortisol-induced catabolism. The American Veterinary Medical Association recommends structured quality-of-life (QoL) scales to guide owner decisions about treatment continuation or euthanasia.
Seven-Factor Quality of Life Assessment
|
Factor |
Poor (0–3) |
Moderate (4–6) |
Good (7–10) |
|
Hurt / pain |
Visible distress, vocalizing |
Occasional discomfort |
No pain signs |
|
Hunger |
Refuses food |
Eats with coaxing |
Eats normally |
|
Hydration |
Dehydrated, sunken eyes |
Drinks adequately |
Normal thirst balance |
|
Hygiene |
Soiled, mat-ridden coat |
Needs assistance |
Clean, intact skin |
|
Happiness |
Withdrawn, unresponsive |
Limited engagement |
Tail-wagging, interactive |
|
Mobility |
Cannot stand |
Walks with weakness |
Moves comfortably |
|
More good days than bad |
Bad days dominate |
Equal balance |
Good days dominate |
The Royal Veterinary College VetCompass team developed the Cushing’s Clinical Score (CCS), a standardized instrument used during consultations to track treatment response. The CCS is freely downloadable from the RVC VetCompass website.
When Should Euthanasia Be Considered for Dogs with Cushing’s Disease?
Euthanasia should be considered when quality-of-life scores remain below 4/10 across multiple factors for 5–7 consecutive days despite maximum therapy. The AVMA’s end-of-life guidelines prioritize comfort, dignity, and relief from refractory suffering over lifespan extension.
Nine Clinical Indicators Supporting Euthanasia
- Complete anorexia exceeding 72 hours.
- Collapse episodes occurring more than once daily.
- Refractory urinary infections unresponsive to sequential antibiotic courses.
- Chronic dermatitis and pressure sores from recumbency.
- Inability to stand, walk, or reposition independently.
- Neurological decline including cluster seizures or circling.
- Concurrent diabetic ketoacidosis or Addisonian crisis.
- QoL scores below 4/10 sustained for 5+ days.
- Absence of moments of joy, play, or family recognition.
See also: When to Euthanize a Dog with Cushing’s Disease — Decision Guide
Owner Experiences Managing Canine Cushing’s Disease
Managing a dog with Cushing’s disease requires consistent medication timing, structured bathroom access, dietary discipline, and routine veterinary monitoring. The Royal Veterinary College’s Big Canine Cushing’s Project collects owner-reported outcomes through structured surveys to quantify day-to-day disease impact.
Internal link: How Owners Managed Their Dog’s Cushing’s Disease — Real Cases
Frequently Asked Questions About Cushing’s Disease in Dogs
Is Cushing’s disease in dogs painful?
Cushing’s disease itself is not painful because cortisol does not activate pain receptors. Secondary complications including calcinosis cutis, pyoderma, urinary tract infections, and pancreatitis produce discomfort requiring separate management.
Can Cushing’s disease cause seizures in dogs?
Seizures occur in approximately 5–10% of Cushing’s cases when a pituitary macroadenoma expands beyond 10 mm and compresses adjacent brain tissue. Concurrent diabetes mellitus and systemic hypertension also contribute to seizure risk.
What breeds are most prone to Cushing’s disease?
The Bichon Frise carries the highest odds ratio at 6.17, followed by the Border Terrier at 5.40 and the Miniature Schnauzer at 3.05, according to the 2021 Royal Veterinary College VetCompass study. Median diagnosis age is 10.9 years.
What is the cost of treating Cushing’s disease in dogs?
Trilostane therapy costs $50–150 monthly, ACTH stimulation monitoring costs $100–200 every 3 months, adrenalectomy surgery ranges $2,000–6,000, and stereotactic radiation costs $2,000–5,000. First-year total costs typically fall between $1,200 and $8,000 depending on the chosen protocol.
What foods are recommended for dogs with Cushing’s disease?
Veterinary diets with less than 12% fat, 18–25% protein, and 5–10% fiber preserve muscle mass and reduce pancreatitis risk. Lean proteins such as turkey breast, white fish, and egg whites pair with soluble fibers from pumpkin and green beans.
How long do dogs live after a Cushing’s diagnosis?
Dogs with pituitary-dependent Cushing’s treated with twice-daily low-dose trilostane have a median survival of 998 days, according to a 2022 Veterinary Record study. Untreated dogs survive 6–24 months depending on concurrent diseases and tumor type.
Can Cushing’s disease be cured in dogs?
Adrenal-dependent Cushing’s caused by a benign unilateral adrenal adenoma can be cured through adrenalectomy. Pituitary-dependent Cushing’s is managed rather than cured because trilostane suppresses cortisol synthesis without eliminating the pituitary adenoma.
What is atypical Cushing’s disease?
Atypical Cushing’s disease produces elevated adrenal sex hormones (17-OH progesterone, androstenedione, estradiol) with normal cortisol on ACTH stimulation. Diagnosis requires an adrenal sex hormone panel, and treatment centers on melatonin and flaxseed lignans rather than trilostane.
Scientific Sources Referenced in This Article:
- Schofield, I., et al. (2021). Frequency and risk factors for naturally occurring Cushing’s syndrome in dogs attending UK primary-care practices. Journal of Small Animal Practice, VetCompass Programme, Royal Veterinary College.
- García San José, P., et al. (2022). Survival of dogs with pituitary-dependent hyperadrenocorticism treated twice daily with low doses of trilostane. Veterinary Record.
- Systematic Review and Meta-Analysis (2025). Effectiveness of Medical Treatment on Survivability in Canine Cushing’s Syndrome. Animals, MDPI.
- Fracassi, F., et al. (2019). Cushing’s syndrome — an epidemiological study based on a canine population of 21,281 dogs. Open Veterinary Journal, University of Bologna.
- Schofield, I., et al. (2020). Development and internal validation of a prediction tool to aid the diagnosis of Cushing’s syndrome in dogs. Journal of Veterinary Internal Medicine.
- Miceli, D. D., et al. (2023). Effects of concurrent canine Cushing’s syndrome and diabetes mellitus on insulin requirements, trilostane dose, and survival time. Research in Veterinary Science.
- American College of Veterinary Internal Medicine (ACVIM) Consensus Statement on Canine Hyperadrenocorticism.
- Cornell University College of Veterinary Medicine — Endocrinology Service.
- American Veterinary Medical Association (AVMA) End-of-Life